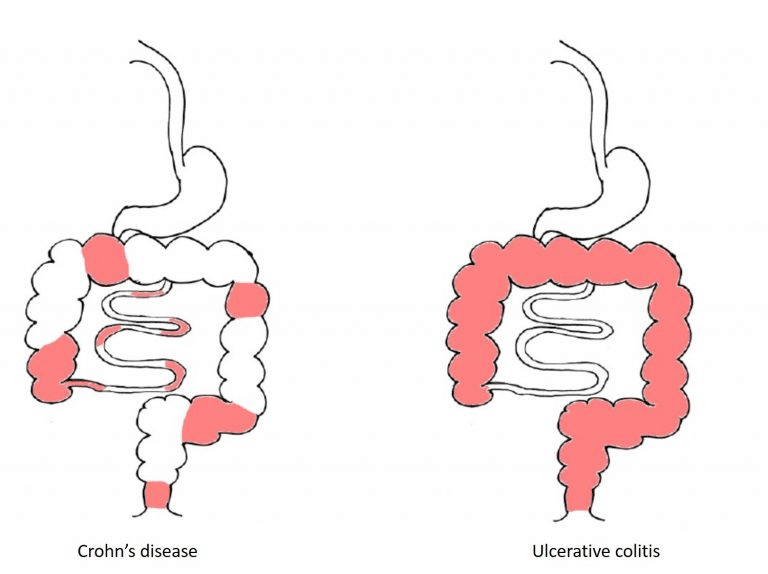
Inflammatory Bowel Disease (IBD) are chronic diseases characterized by inflammation of the intestines (your gut). Crohn’s disease (CD) can involve any part of the intestinal tract from “gum to bum”, while ulcerative colitis (UC) involves the large intestine (colon) only.
Although the exact cause of IBD is unclear, scientists have determined that risk factors include genes, environment (diet, smoking, pollution), microbiome (bacteria), and immune system.
IBD is not the same as IBS (irritable bowel syndrome) although people with IBD can have IBS as well. IBS does not have the inflammation and ulceration that IBD has, although people with IBS can have similar symptoms of cramps, diarrhea, constipation. People with IBS however should not have the red alarm symptoms of blood from the rectum, or weight loss.
IBD is a chronic disease, with no cure at this time. Researchers around the world continue to study the causes or risk factors for IBD, as well as treatments for IBD. Most people with IBD take medications to control the inflammation. Some patients need surgery to remove diseased portions of their intestines or to manage complications of IBD such as strictures or fistulas.
Watch our Intro to IBD video below for more information:
People with IBD can have complications of the disease. Crohn’s disease is commonly complicated by strictures, fistulas, and abscess.
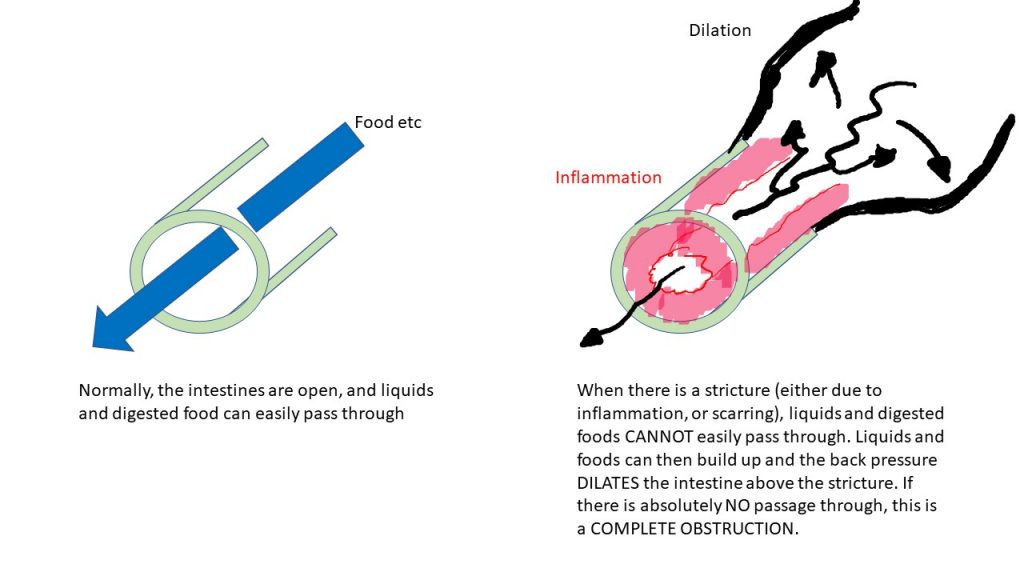
A stricture is a narrowed section of the intestine – think of a clogged garden hose or a sewer pipe. When there is narrowing, the flow of liquids and food through the intestine is slower, and in some cases can be blocked or obstructed. In severe cases, surgery is required to remove the stricture or to open the stricture.
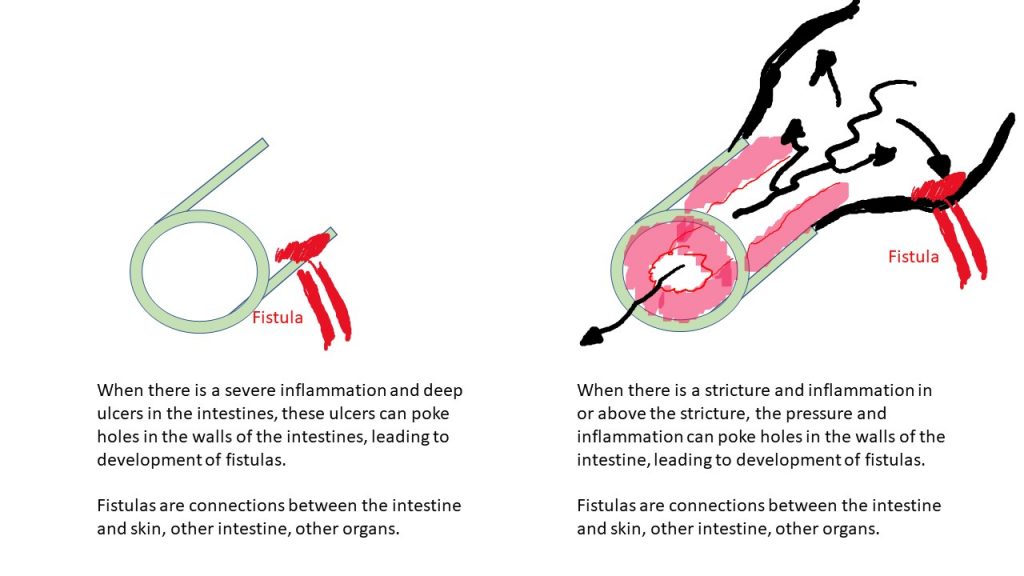
A fistula is a connection between the intestine and another organ (another part of the intestine, to the skin around the bum, to the skin on the abdomen, to other organs). Fistulas typically develop from an ulcer that has gone through the intestinal wall, and can be associated with abscesses (infected fluid collections). Strictures can drive fistulas – meaning the pressure of the backed up fluids and food contents above the stricture, can push outwards to any weakened or ulcerated area, leading to the fistula. For example, think of a very old “garden hose” that you use to water your lawn. If the “garden hose” (ie intestine) has weakened areas (ie ulcers) or already has holes (ie perforations) in it, and you “pinch” or “block” (ie narrowing, stricture) the water flow –> the water above the “pinched” or “blocked” area will build up pressure, and the water will find the weakest spot or the holes that already exist, and thus you have a “leaking” garden hose! Your body will try to heal itself, and most often ends up creating connections (ie fistulas) from the diseased area, to another area of intestine, or to the skin, or another organ.
Perianal disease refers to inflammation around the anus (where you pass stool). This can include abscesses, fistulas, skin tags.
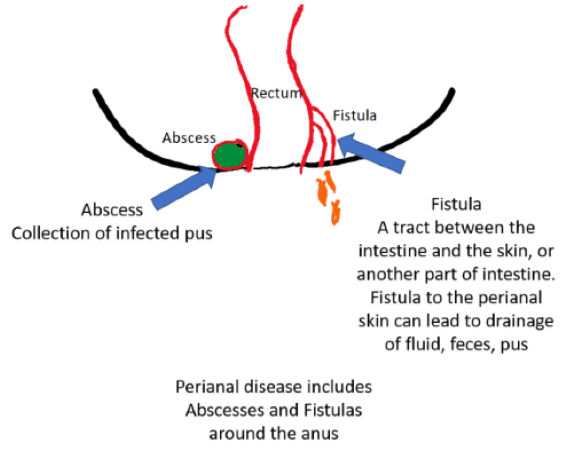
An abscess is a collection of infected fluid or pus. Abscesses need to be treated with antibiotics and sometimes drained surgically.